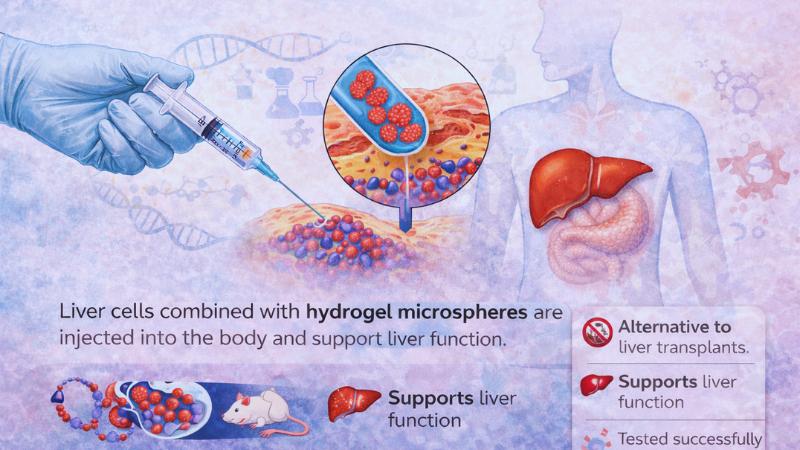
Scientists at the Massachusetts Institute of Technology (MIT) have developed a groundbreaking approach to treating liver failure with the creation of injectable "satellite livers." These tiny engineered liver tissues, which combine liver cells (hepatocytes) with hydrogel microspheres, offer a potential solution to the global shortage of donor livers. Instead of undergoing a complex transplant surgery, patients could receive these miniature tissue grafts as an injectable treatment that assists in performing the critical functions of the liver.
The liver, one of the most vital organs in the human body, performs more than 500 essential functions such as filtering toxins from the bloodstream, producing proteins, and aiding digestion. When the liver fails, a transplant is often the only life-saving option. However, donor organs are limited, and many patients are either too weak for surgery or unable to find a matching donor. In response to these challenges, MIT engineers have explored alternative methods, developing lab-grown tissues that could temporarily support liver function.
The "satellite liver" technology involves a mixture of liver cells and hydrogel microspheres, created using a microfluidic device. This gel-like substance allows the liver cells to survive and grow when injected into the body. The microspheres form a stable environment in which the cells can perform their functions, similar to the behavior of a natural liver. In laboratory experiments with mice, these grafts were injected into fatty tissue in the abdomen and were able to survive for at least eight weeks, producing vital liver proteins and enzymes during that time.
Researchers believe that these mini grafts could serve as a "biological backup system" for people with liver failure. Unlike traditional liver transplants, the satellite livers wouldn't replace the damaged organ; instead, they would act as additional functional tissue, sharing the workload with the failing liver. This injectable therapy could serve two important roles: as an alternative for patients who cannot undergo a transplant and as a temporary support mechanism for those waiting for a donor organ. Since the grafts are injectable, they can be added later if additional support is needed, offering flexibility in treatment.
Another advantage of this new approach is that the grafts do not need to be placed directly into the liver. As long as the liver cells have access to blood vessels and sufficient space, they can function in various areas of the body, such as fatty tissue in the abdomen, the spleen, or near the kidneys. This added flexibility makes the therapy easier to administer.
Despite its promising potential, one major challenge remains: the immune system’s response to foreign cells. Patients may need to take immunosuppressive drugs, similar to those used after organ transplants, to prevent their bodies from rejecting the grafts. To address this, researchers are exploring strategies to create "stealth" liver cells that can avoid immune detection, or using the hydrogel itself to slowly release immunosuppressive drugs around the grafts.
Although this technology has only been tested in mice, it represents a promising step forward in treating liver failure and reducing the dependence on organ transplants. If successful in humans, these injectable satellite livers could revolutionize the treatment of chronic liver diseases, offering a temporary or long-term solution for patients who otherwise would have limited options. This innovation could ultimately help thousands of people around the world who are living with liver disorders and are waiting for life-saving transplants.




































