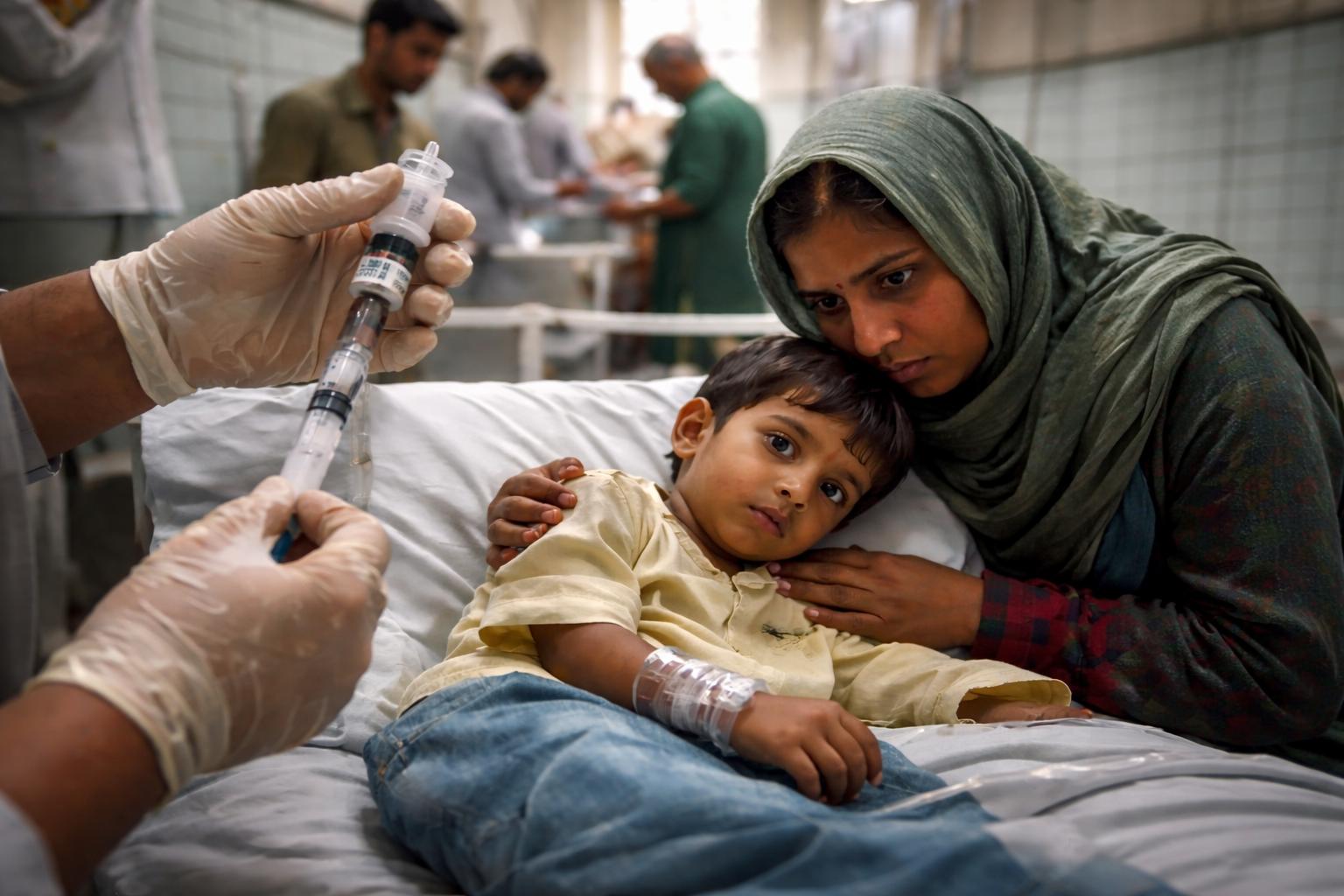
An undercover investigation by the BBC has uncovered alarming medical negligence at a government hospital in Taunsa, Punjab province, Pakistan, which is believed to be linked to a deadly HIV outbreak among children. Between November 2024 and October 2025, at least 331 children in Taunsa tested positive for HIV, sparking serious concerns about the hospital’s unsanitary practices, including the reuse of syringes and improper handling of medical waste.
The shocking footage captured during the investigation shows repeated violations of infection control protocols at Tehsil Headquarters (THQ) Hospital, where syringes were reused on multiple children and medical staff administered injections without sterile gloves. The investigation highlighted how the use of contaminated syringes may have exposed hundreds of children to HIV, with a significant number of families suspecting that their children contracted the virus during routine medical treatment.
Among the victims were eight-year-old Mohammed Amin and his sister Asma, who were both diagnosed with HIV after receiving injections at the same hospital. Mohammed passed away shortly after his diagnosis, and Asma now faces lifelong treatment for HIV. Both children’s mother tested negative for the virus, raising suspicions that unsafe medical practices at the hospital were to blame.
A provincial screening program indicated that contaminated needles were the primary mode of transmission for over half of the affected children, further supporting the link between the hospital’s practices and the HIV outbreak. Medical experts reviewing the footage confirmed that reusing syringes, even with new needles, still poses a risk of contamination, making the practices at THQ Hospital highly dangerous.
Despite the damning evidence, the hospital’s medical superintendent denied any wrongdoing, questioning the authenticity of the footage. Previous promises from the government to address the unsafe practices at the hospital were not followed through, and unsafe practices continued for months after the initial reports surfaced. A joint review by the World Health Organization (WHO) and UNICEF also flagged severe lapses in infection control at local health facilities, citing the reuse of intravenous equipment and poor hygiene.
This case reflects broader systemic issues within Pakistan’s healthcare system, including the overuse of injections, shortages of medical supplies, and a lack of proper training for healthcare workers. Pakistan has one of the highest rates of therapeutic injections globally, many of which are unnecessary, contributing to the ongoing healthcare crisis.
The repercussions for the affected families have been devastating. Asma, now living with HIV, faces both lifelong medical treatment and the stigma associated with the disease. Her family shares the emotional toll of social isolation, as neighbors avoid her, leaving her isolated and questioning her condition. The ongoing investigation and the tragic human cost of this outbreak serve as a stark reminder of the pressing need for reform in Pakistan’s healthcare practices to prevent further outbreaks and protect vulnerable populations.